Are Independent Medical Evaluation (IME) Providers Really "Independent"?
After being twice denied continued disability benefits, an Addiction Medicine Physician, with the help of his California Disability Attorney, was forced to file a lawsuit against Hartford.
Dr. K has been employed by Loma Linda University School of Medicine (“Loma Linda”) as an Addiction Medicine Physician. In June 2007, Dr. K was forced to leave work due to acute myocardial infarction and severe coronary artery disease. After undergoing a quintuple bypass surgery, Dr. K. made a claim with Hartford, his disability insurance carrier, and was paid short-term disability (“STD”) insurance benefits followed by long-term disability (“LTD”) benefits.
This is a case about the relationship between a disability insurance company and its allegedly “independent” third party IME providers.
Hartford terminates payments of LTD benefits
In February 2009, Dr. K was notified by letter from a Hartford Investigative Specialist, that he no longer satisfied the definition of disability under the policy. As a result, Hartford denied further disability benefits payments to Dr. K.
Dr. K. appealed Hartford’s decision to terminate his LTD benefits. Two months later, Hartford denied Dr. K’s appeal. With his administrative remedies exhausted, Dr. K was forced to file a lawsuit against the Hartford. (View more information and other similar cases involving The Hartford).
Court finds Hartford was wrong
Following his unsuccessful appeal, Dr. K and his California disability attorney sued Hartford in a California court. After reviewing the record, the court concluded that Hartford’s decision was wrong.
When conducting a review of Dr. K’s claim, Hartford had lingering questions regarding Dr. K’s functionality. Instead of arranging for a Functional Capacity Evaluation (“FCE”), Hartford referred Dr. K’s claim to MES Solutions and UDC – two companies with which Hartford has long, well-established relationships. In fact, as the court later discovered, both companies relied heavily on Hartford for a sizeable portion of their overall revenues.
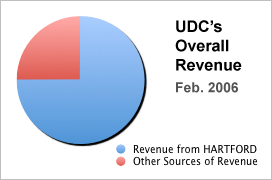
From the end of 2004 to February 2006, Hartford referred to UDC an average of 200 to 250 claims per month. By February 2006, UDC derived 70-75 percent of its overall revenue from Hartford.
From 2007 to 2009, the year when Dr. K’s benefits were terminated, Hartford referrals to MES increased from 673 to 1,496 claims and the amount billed by MES for these referrals almost tripled – from about $.5 million in 2007 to roughly $1.5 million in 2009.
As the court explained, these numbers cast doubts on the reliability of the claim reviews done by UDC and MES as well as Hartford’s decision to terminate Dr. K’s benefits. The court explained that the nature of Hartford’s relationship with UDC and MES creates an incentive for the companies to reach results that are favorable to Hartford in order to keep their business. In other words, UDC and MES both had strong motivations to support the denial of Dr K’s claim.
Accordingly, the court was unconvinced UDC and MES had provided an unbiased review of Dr. K’s claim and concluded that Hartford had failed to conduct a full and fair review of Dr. K’s claim.
Resources to Help You Win Disability Benefits
Submit a Strong Hartford Appeal Package
We work with you, your doctors, and other experts to submit a very strong Hartford appeal.
Sue Hartford
We have filed thousands of disability denial lawsuits in federal Courts nationwide against Hartford.
Get Your Hartford Disability Application Approved
Prevent a Hartford Disability Benefit Denial
Negotiate a Hartford Lump-Sum Settlement
Our goal is to negotiate the highest possible buyout of your long-term disability policy.
Policy Holder Rating
Former Hartford employee has had life insurance and accidental death policy's revoked for one late premium payment
Reply
Bad Faith
Denied by Hartford after 20 years of Payments
This company is a scam!
Hartford Stopped Payments
Hartford never paid me
Reply
Hartford rep felt so guilty over how the company treated me that she quit
Reply
Hartford ajuster won't return my calls. I might have to move back to California
Q: Disability company dropped my monthly benefits
Q: The Hartford stopped monthly benefits for repayment due to an overpayment. Once monthly benefits end do I still have to repay remaining overpayment balance?
Q: Short term vs long term
Q: After 3 months my LTD approval, insurance company stopped LTD payment during review of continuity and also have argument with insurance company regarding offset of my son's disabled adult child benefits
Q: Can I do anything to get my LTD ?
Q: Lifetime disability policy with Hartford
Q: Can the Hartford reduce my long term disability payment due to a rental income?
Q: Is there a specific video to help me prepare for a Hartford doctor appointment (IME)?
Does Hartford Pay Disability Insurance Claims?
How Does Hartford Long Term Disability Work?
What Happens If My Hartford Short Term Disability Claim is Denied?
How Long Does a Hartford Short Term or Long Term Disability Claim Last?
If I Convert my Former Employee Disability Policy to a Private Policy Does ERISA Govern?
Is the Hartford Disability Purchase of Aetna Bad for Aetna LTD Policy Holders?
Hartford Disability Claim Problems
How Can I Protect Myself At A Hartford IME Exam?
Nurse With Knee and Back Disorder Wins Hartford Disability Appeal
Executive Director with Meniere's Denied Long Term Disability Insurance Benefits By Hartford
A Hartford Disability Benefit Lawsuit Victory for Truist Banker with Lupus
Hartford Denies Disability Benefits To Home Depot Employee 3 Weeks Before Change of Disability Definition
Hartford Denies Long Term Disability Benefits After Paying for 22 Years
Hartford Overturns Denial of Disability Benefits on Appeal
Hartford Approves Disability Claim After Appeal Deadline
Hartford overturned its previous denial of LTD benefits for Illinois Account Representative
Reviews from Our Clients







